Are Ingrown Toenails Really “Ingrown”?
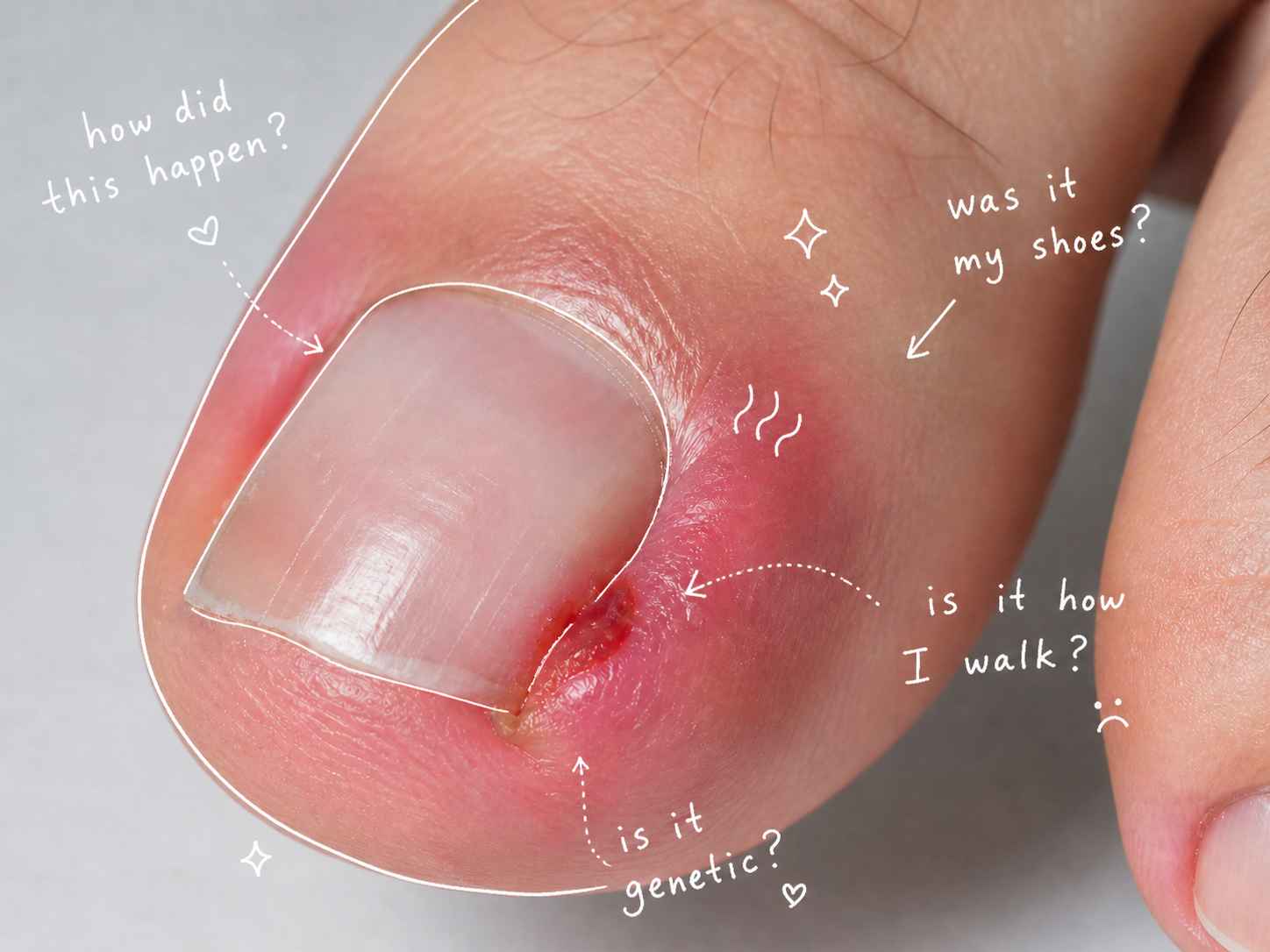
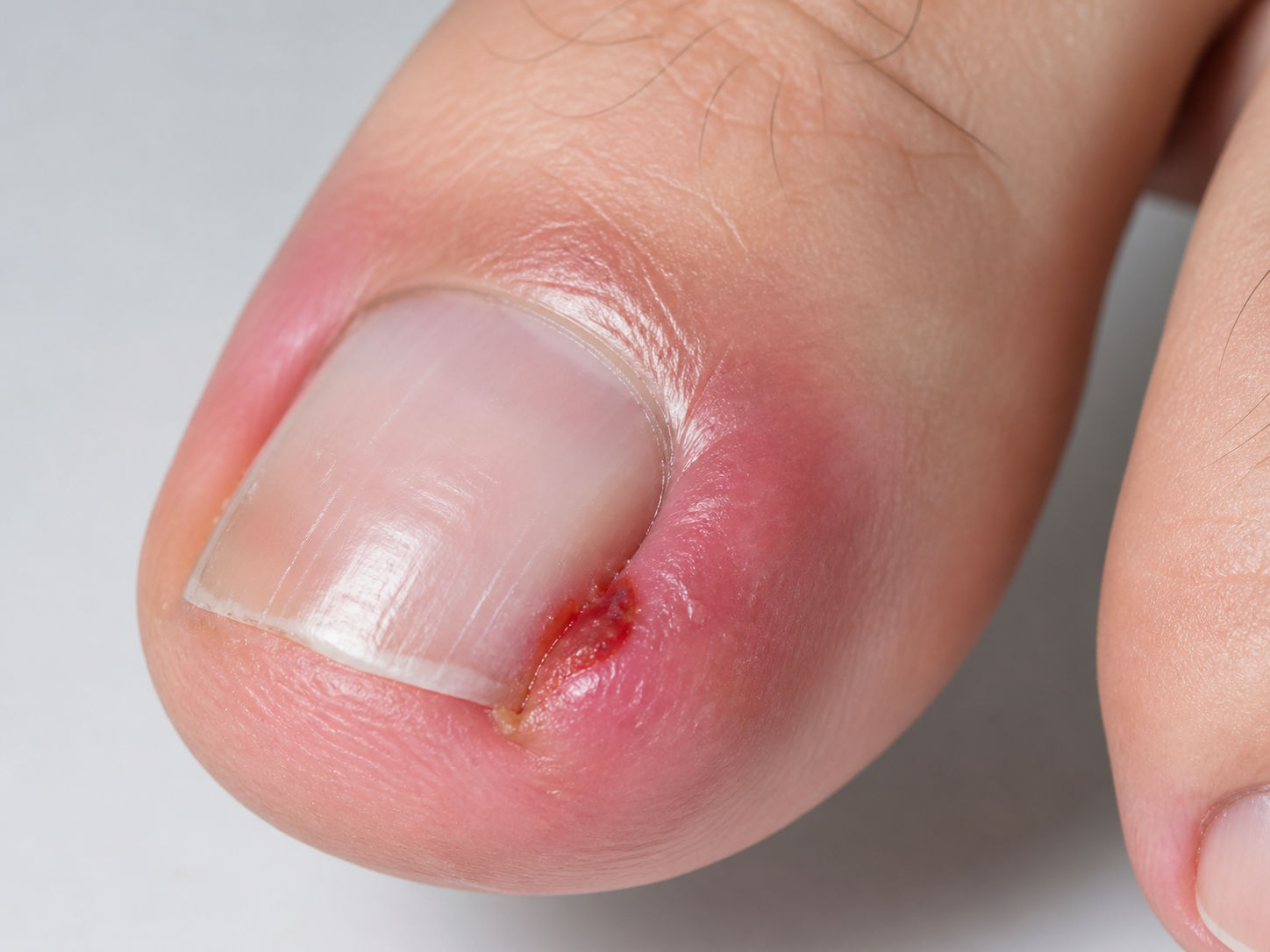
An ingrown toenail sounds simple: the nail grows into the skin. But clinically, the story is more interesting. In many cases, the nail is not behaving like a plant root growing into tissue. Instead, an “ingrown” toenail is often a mechanical conflict between the nail plate, the nail fold, the toe, the shoe, and the ground.
The medical term for an ingrown toenail is onychocryptosis, from the Greek words for “nail” and “hidden”. It most commonly affects the big toe and can cause pain, swelling, inflammation, discharge, infection and difficulty walking (Khunger and Kandhari, 2012). The usual description is that the edge of the nail plate penetrates or irritates the lateral nail fold, creating inflammation and sometimes granulation tissue (Khunger and Kandhari, 2012). But this description can make it sound as though the nail alone is the villain.
In reality, the condition is usually a biomechanical interface problem.
The nail may be normal. The skin may be normal. But when pressure, rotation, poor nail trimming, footwear compression, toe alignment and ground reaction forces act repeatedly on the same small area, the nail edge and the nail fold can begin to injure one another.
Is the nail really growing into the skin?
Sometimes, yes. A sharp nail spike can pierce the nail fold. This may happen after the nail has been cut too short, rounded at the corners, torn, split or damaged. Once a small nail spicule is left behind, the advancing nail edge can act like a tiny rigid wedge against soft tissue (Khunger and Kandhari, 2012).
But in many patients, the phrase “ingrown toenail” is slightly misleading. The problem may be less about the nail “growing into” the skin and more about the skin being compressed, swollen or pushed up against the nail edge.
This distinction is important. Khunger and Kandhari (2012) describe the ongoing controversy in the literature: is the primary fault the nail plate, or is it the soft tissue around the nail? One theory proposes that excess tissue beside the nail bulges around the nail during weightbearing, creating pressure, tissue breakdown and inflammation. A prospective study by Pearson et al. (1987) found no consistent abnormality in nail shape among patients with symptomatic ingrown toenails, suggesting that treatment should not always be based on the assumption that the nail itself is deformed.
That idea changes how we think about the condition. The nail may not always be “growing badly”. The toe may be experiencing bad mechanics.
The nail unit is a pressure-bearing structure
The toenail is not just a cosmetic plate. It is part of the functional anatomy of the toe.
When we walk, the big toe stabilises the forefoot, helps the body progress forward and contributes to propulsion. During late stance and toe-off, load passes through the hallux. The soft tissue beneath and around the nail is exposed to repeated compression, shear and bending forces.
The nail plate helps resist deformation of the pulp of the toe. It provides a firm dorsal counter-surface, allowing the pulp of the toe to press against the ground without simply spreading upward and outward. In this sense, the nail and soft tissue form a small mechanical unit.
This is why ingrown toenails are not only a dermatological problem. They are also a load-transfer problem.
Book An Appointment
Book An Appointment
The key biomechanical forces behind ingrown toenails
Several mechanical forces can contribute to onychocryptosis. These forces rarely act alone.
1. Medial-lateral compression from footwear
Tight shoes, narrow toe boxes, safety boots, football boots, court shoes and fashion footwear can compress the great toe from side to side. Khunger and Kandhari (2012) describe poorly fitting shoes as an important factor, explaining that tight footwear can place direct pressure on the medial nail wall and indirect pressure on the lateral wall as the big toe is pushed against the second toe.
This matters because the nail plate is relatively rigid, while the nail fold is soft. If the shoe compresses the toe, the soft tissue can be squeezed against the nail edge. Over time, this can create inflammation, tenderness and sometimes tissue breakdown.
In this model, the nail is not necessarily growing incorrectly. The shoe is narrowing the available space, and the nail fold is being forced into the nail.
2. Ground reaction force and soft-tissue bulging
Every step creates ground reaction force under the toe. During propulsion, the pulp of the hallux is compressed between the ground and the distal phalanx. As soft tissue is compressed, it can expand into available spaces.
If the lateral or medial nail fold is bulky, swollen, macerated or repeatedly irritated, weightbearing may cause it to bulge around the nail margin. Khunger and Kandhari (2012) specifically describe the theory that wide tissue beside the nail can bulge around the nail during weightbearing, leading to pressure necrosis.
This explains why some patients feel worse when standing, walking, running or wearing closed shoes. The “ingrowing” event may be dynamic: the tissue and nail collide more aggressively under load.
3. Shear force during walking and sport
Walking is not pure vertical loading. The toe also experiences shear.
As the body passes over the foot, the hallux may rotate, abduct, adduct or press against adjacent toes. In sport, especially activities with cutting, stopping, jumping or kicking, the hallux can be forced repeatedly into the end or side of the shoe.
These repetitive shear forces can irritate the nail fold and create small breaks in the skin. Once the skin is inflamed, swollen or macerated, the mechanical relationship worsens. A nail edge that was previously tolerated can become painful because the soft tissue has expanded into its path.
This is why ingrown toenails are common in teenagers and young adults, especially active individuals. Khunger and Kandhari (2012) note that adolescents may be predisposed by increased perspiration, sports participation and nail spicule formation.
4. Nail trimming changes the shape of the mechanical edge
Poor nail cutting is one of the most commonly cited causes of ingrown toenails. Cutting the nail too short or rounding the corners can create a sharp residual edge. As the nail grows forward, that edge can behave like a spike (Khunger and Kandhari, 2012).
Biomechanically, this changes the nail from a smooth, broad plate into a pointed lever.
A straight nail edge distributes contact more evenly. A small nail spike concentrates force into one point. That concentrated force can penetrate or irritate the nail fold, particularly when shoe pressure and ground reaction force are added.
This is why patients often report that the problem began after “digging out” the corner of the nail. The relief may be temporary, but the remaining nail edge may grow forward as a sharper, deeper spicule.
5. Hyperhidrosis and maceration weaken the soft tissue
Excessive sweating does not simply make the foot damp. It changes tissue behaviour.
Macerated skin is softer and less resistant to penetration. Khunger and Kandhari (2012) describe excessive sweating and maceration as factors that soften the nail folds, making them easier for the nail to penetrate.
From a biomechanics perspective, this is a material-property problem. The nail plate remains relatively firm, while the surrounding skin becomes softer and more vulnerable. Under the same amount of pressure, softened tissue deforms more and is more easily injured.
This may partly explain why ingrown toenails can be common in people who wear enclosed shoes for long hours, athletes, military personnel and those in humid climates.
Book An Appointment
Book An Appointment
Toe alignment: why the direction of the toe matters
The big toe is not always pointing straight ahead. Hallux valgus, hallux interphalangeus, distal phalanx deviation, pes planus and forefoot abduction may all alter the way force passes through the toe.
This area of research is still developing, and studies are not perfectly consistent.
Darwish et al. (2008) investigated whether abnormal hallux valgus and interphalangeal angles were associated with onychocryptosis. Later, Kim et al. (2022) studied young military patients and found that a lower medial longitudinal arch appeared to be a predisposing factor for ingrown toenail development, while lateral nail fold involvement was associated with lateral deviation of the distal phalanx. Their study also noted that patients with ingrown toenails had radiographic features reflecting lower arch alignment and forefoot abduction, although the relationship is not simple.
This supports a biomechanical hypothesis: if the hallux is deviated, rotated or loaded asymmetrically, one side of the nail fold may be exposed to greater pressure.
However, not all studies agree. Sarı et al. (2024) found no significant difference in several hallux valgus and pes planus radiographic measurements between patients with ingrown nails and controls, although they did report a moderate relationship between ingrown nail stage and talometatarsal angle for pes planus diagnosis.
This does not mean biomechanics is irrelevant. It means that ingrown toenails are probably multifactorial, and static X-rays may not capture all the dynamic forces that occur during gait, footwear use and sport.
The lower arch hypothesis
The Kim et al. (2022) military study is particularly interesting because it attempted to reduce confounding factors. Military trainees are often similar in age, activity exposure and footwear. In that cohort, a lower medial longitudinal arch appeared to predispose to ingrown toenail development.
How might a lower arch contribute?
A lower arch is often associated with increased pronatory mechanics, greater forefoot abduction and altered hallux loading. If the forefoot abducts and the hallux is repeatedly compressed or rotated against the shoe or second toe, the nail fold may receive more asymmetrical pressure.
This does not mean every flat foot causes ingrown toenails. It means that in some patients, the ingrown toenail may be the small visible symptom of a larger mechanical loading pattern.
In other words, the painful nail edge may be the endpoint of abnormal force distribution.
The Big and second toe relationship
The hallux does not function in isolation. It sits beside the second toe inside a confined shoe.
Kose et al. (2011) proposed that biomechanical imbalance between the hallux and second toe, along with external compression of the lateral nail fold, could contribute to ingrown toenails. Their case-control study did not demonstrate a clear abnormality in forefoot alignment in patients with symptomatic ingrown toenails, showing again that this topic is complex and not reducible to a single angle or deformity.
Clinically, however, the concept remains useful: when the hallux is pushed against the second toe, the lateral nail fold can become trapped between the nail plate, the second toe and the shoe upper.
That is a mechanical sandwich: nail on one side, shoe or adjacent toe on the other, soft tissue in between.
Book An Appointment
Book An Appointment
The nail fold may be the “victim” and the “driver”
Once inflammation begins, the nail fold becomes swollen. Swelling increases tissue volume. Increased tissue volume makes the fold press even more against the nail. More pressure creates more inflammation.
This creates a self-reinforcing cycle:
pressure → irritation → swelling → more pressure → more nail-fold conflict
At this stage, the nail may appear to be deeply embedded, but part of the problem is that the surrounding tissue has enlarged around it. This is why some surgical approaches focus not only on narrowing the nail but also on reducing or reshaping hypertrophic nail-fold tissue.
Are curved nails always the cause?
No.
A highly curved nail plate, including a pincer-type nail, can certainly increase risk because the nail edge points more aggressively into the nail groove. Khunger and Kandhari (2012) note that a nail curved from side to side may be more likely to become ingrown, especially in severe pincer nail forms.
But curvature alone is not the whole story. Pearson et al. (1987) found no consistent nail-shape abnormality in symptomatic ingrown toenail patients, which challenged the assumption that the nail plate is always the primary defect.
This is clinically important. A patient may have a normal-looking nail but abnormal mechanical loading. Another patient may have a curved nail but no symptoms because the surrounding forces are favourable.
The pathology appears when the relationship between nail, skin and force becomes pathological.
Why recurrence happens
Recurrence often occurs when the visible nail edge is treated but the underlying mechanical environment remains unchanged.
For example, a patient may have the painful nail spike removed, but continue to wear narrow shoes, continue cutting the nail corners too short, continue playing sport in tight footwear, or continue loading the hallux asymmetrically.
This helps explain why ingrown toenails can become chronic. The nail grows back into the same mechanical conflict zone.
Treatment may therefore need to address both the nail and the forces acting on it.
Practical biomechanical prevention principles
For patients prone to ingrown toenails, prevention should focus on reducing the mechanical conflict between the nail edge and nail fold.
This means:
- Avoid narrow toe boxes that compress the big toe.
- Avoid repeatedly cutting down the nail corners.
- Cut the nail straighter across, leaving the corners visible.
- Use footwear with enough depth and width around the toes.
- Be careful with tight sports shoes, football boots, court shoes and safety shoes.
- Manage excessive sweating and maceration.
- Seek early care when the nail fold becomes painful, swollen or red.
- Consider foot mechanics if the problem is recurrent, especially where there is hallux deviation, flatfoot mechanics or repeated pressure on one side of the big toe.
The goal is not simply to “stop the nail growing in”. The goal is to reduce the repeated pressure that makes the nail and skin collide.
Conclusion: “ingrown” is a useful term, but not the whole truth
Ingrown toenails are real, painful and sometimes infected conditions. But the word “ingrown” can oversimplify the pathology.
In many patients, the nail is not mysteriously growing into the toe. Instead, the toe is caught in a small but powerful biomechanical conflict. Footwear compression, nail cutting, toe alignment, ground reaction force, soft-tissue bulging, sweating, sport and repetitive trauma can all contribute to the nail-fold injury.
So, are ingrown toenails really ingrown?
Sometimes. But very often, they are better understood as mechanically driven nail-fold impingement.
That distinction matters because it shifts the clinical focus from the nail alone to the entire environment around the nail: the toe, the shoe, the skin, the gait pattern and the forces of daily walking.
If you are suffering form ingrown toenails and would like to see us book here.
Disclaimer: The word "treatment" in this article refers to the care and management of a patient’s health to prevent, cure, or improve a condition. Treatment results vary and do not necessarily indicate a cure. This article is for informational and educational purposes only and does not constitute medical advice.
If you are suffering form ingrown toenails and would like to see us book here.
Disclaimer: The word "treatment" in this article refers to the care and management of a patient’s health to prevent, cure, or improve a condition. Treatment results vary and do not necessarily indicate a cure. This article is for informational and educational purposes only and does not constitute medical advice.
References
8. Thakur, V., Vinay, K. and Haneke, E. (2020) ‘Onychocryptosis: decrypting the controversies’, International Journal of Dermatology, 59(6), pp. 656–669. doi: 10.1111/ijd.14769.
Written and prepared by:
Mark Reyneker
Written and prepared by:
Mark Reyneker
B.T. Pod (SA), MSc (SA)
Podiatrist and Human Gait Specialist
Registered with the Podiatry Association of Singapore
Founder and Director:
Family Podiatry Centre Pte Ltd
Family Podiatry Centre Sdn Bhd
Solescape Orthotics Laboratory
Solescape Shoes brand