Ingrown Toenails - A Comprehensive Guide
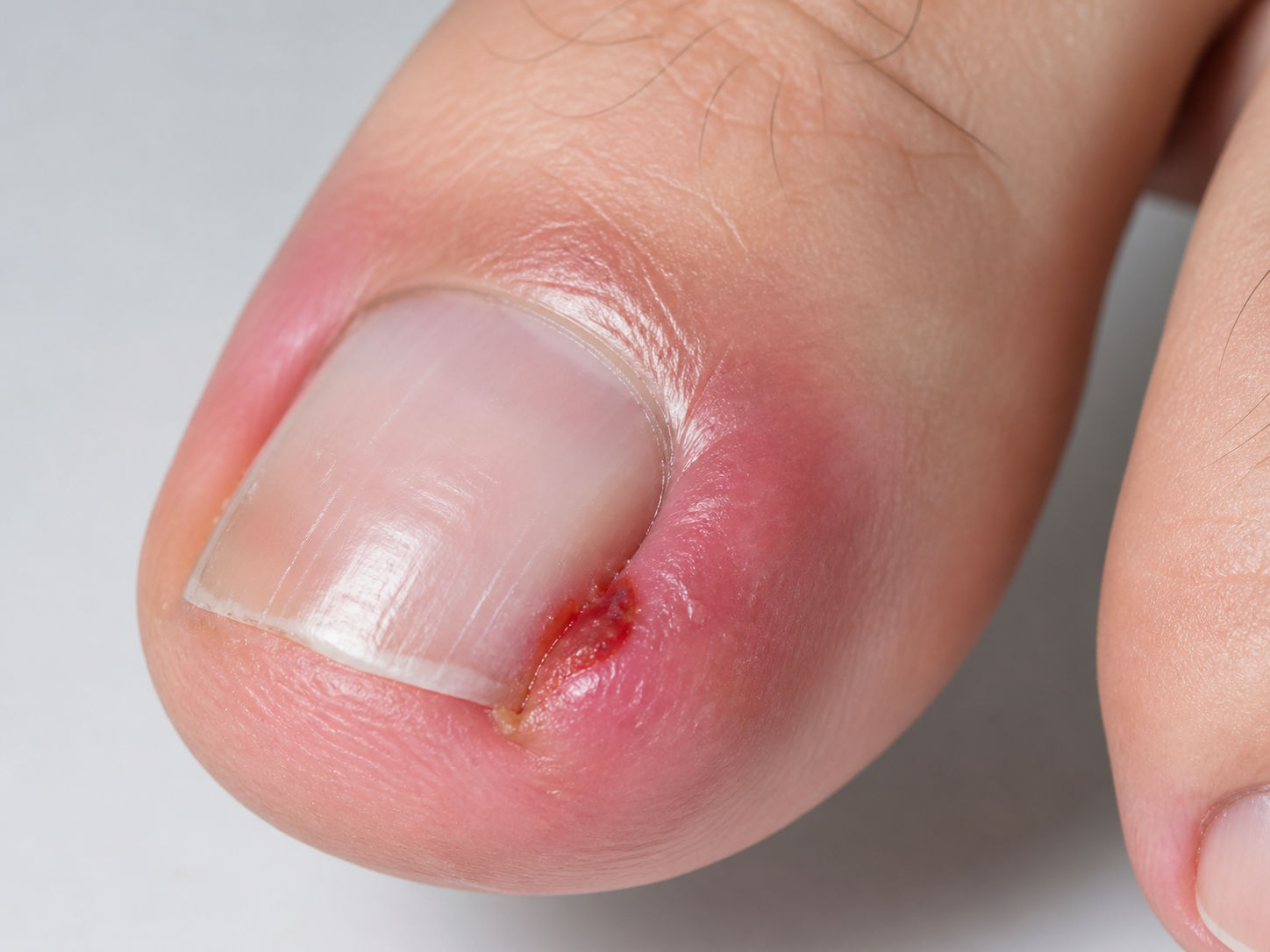
An ingrown toenail, medically called onychocryptosis, is one of the most common painful nail conditions affecting the foot. Although it is often dismissed as a minor problem, it can cause significant pain, difficulty walking, difficulty wearing shoes, recurrent infection, time away from sport, and repeated visits to doctors, podiatrists or emergency clinics.
The condition most commonly affects the big toe, especially along the medial or lateral nail border. At its simplest, an ingrown toenail occurs when the edge of the nail irritates, presses into, or penetrates the surrounding skin fold. However, this simple description does not fully explain why ingrown toenails develop, why they recur, or why some patients respond well to conservative care while others need a surgical procedure.
The current literature suggests that ingrown toenails are best understood as a mechanical conflict between the nail plate and the surrounding soft tissue, influenced by nail shape, nail-cutting technique, footwear, trauma, sweating, sport, body weight, and the anatomy of the nail fold itself (Geizhals and Lipner, 2019; Chabchoub and Litaiem, 2022). The strongest evidence for treatment supports partial nail avulsion combined with destruction of the offending part of the nail matrix, most commonly with phenol, when the condition is recurrent, painful, infected, or associated with excessive granulation tissue (Exley et al., 2023a; Vinay et al., 2022).
What is an ingrown toenail?
An ingrown toenail occurs when part of the nail plate causes injury or chronic irritation to the adjacent nail fold. The nail edge may physically pierce the skin, or the soft tissue may become compressed against the nail until inflammation develops.
The typical clinical features include:
- pain along one or both sides of the nail;
- redness and swelling of the nail fold;
- tenderness when pressure is applied;
- difficulty wearing closed shoes;
- discharge or bleeding in more inflamed cases;
- hypergranulation tissue in chronic or advanced cases.
The term “ingrown toenail” can be slightly misleading because it suggests that the nail is always growing abnormally into the skin. In many cases, however, the problem is not only the nail. The surrounding soft tissue may be swollen, bulky, traumatised, macerated, or inflamed, creating a situation where the nail edge and nail fold repeatedly injure each other.
This is why some clinicians prefer to think of ingrown toenails as a nail–fold conflict, rather than simply a “bad nail”.
Why ingrown toenails happen: the modern etiological model
1. The nail edge and skin fold come into mechanical conflict
The central event in most ingrown toenails is mechanical irritation between the nail plate and the periungual skin. The nail plate is relatively hard, while the adjacent skin fold is soft, vascular, and sensitive. When the nail edge is sharp, curved, too wide for the nail fold, or forced into the tissue by pressure, inflammation can begin.
Once inflammation starts, the nail fold swells. This swelling narrows the space around the nail edge, increasing pressure further. The result is a self-perpetuating cycle:
pressure → irritation → swelling → more pressure → more inflammation → pain and possible infection.
In chronic cases, hypergranulation tissue may develop. This red, friable tissue forms as part of the body’s wound-healing response, but it can make the toe more painful and more prone to bleeding. It also creates a larger soft-tissue mass for the nail edge to press against.
2. Nail-cutting technique can create a nail spicule
One of the most common practical causes of ingrown toenails is poor nail cutting. This does not mean the patient has done something careless; many people are never taught how to cut toenails properly.
Problems arise when the nail is:
- cut too short;
- rounded deeply into the corners;
- torn rather than cut cleanly;
- cut in a way that leaves a sharp nail spike or spicule;
- repeatedly trimmed down the side by the patient to “dig it out”.
A small nail spicule can act like a splinter. As the nail grows forward, the spicule can pierce the lateral nail fold and trigger inflammation.
This explains why many patients describe a cycle where the toe improves temporarily after they trim the painful corner, but the problem returns weeks later. The short-term relief comes from reducing pressure. The recurrence happens because the underlying nail edge or matrix continues to produce the same problematic nail border.
3. Footwear can increase pressure on the nail fold
Shoes with a narrow toe box, shallow upper, tight forefoot, or compressive fit can push the soft tissue against the nail edge. This is especially relevant in patients who wear formal shoes, football boots, dance shoes, court shoes, or fashion footwear with a narrow front.
Footwear is rarely the only cause, but it can be a major aggravating factor. A nail that might otherwise be tolerated can become painful when the toe is repeatedly compressed from the sides or from above.
This is also why some patients report improvement when they wear sandals or open footwear, only for symptoms to return when they resume closed shoes.
4. Sport and repetitive trauma matter
Ingrown toenails are common in active teenagers and young adults. Sports involving sprinting, sudden stopping, kicking, jumping, lunging, and tight footwear can repeatedly traumatise the nail unit.
Examples include:
- football;
- rugby;
- martial arts;
- running;
- tennis;
- netball;
- dance;
- gym training;
- hiking.
Repeated microtrauma can damage the nail fold, bruise the nail plate, or encourage the nail edge to dig into the adjacent tissue. In athletes, sweating and shoe compression often occur together, which can make the nail fold more vulnerable.
5. Hyperhidrosis and maceration soften the nail fold
Sweaty feet are not just a hygiene issue. Excessive sweating can macerate the skin around the nail. Macerated skin is softer, weaker, and more easily damaged by pressure from the nail edge.
This is one reason ingrown toenails are common in adolescents. Teenagers often have higher sweat activity, active lifestyles, school shoes, sports shoes, and sometimes less consistent nail care.
Hyperhidrosis is repeatedly mentioned in reviews as a risk factor for onychocryptosis (Geizhals and Lipner, 2019).
6. Body weight and soft-tissue pressure may contribute
Body weight may influence ingrown toenails by increasing load through the forefoot and toes. Increased pressure may expand or compress the periungual soft tissue against the nail edge.
This does not mean ingrown toenails are simply caused by weight. Thin, athletic patients can develop severe ingrown toenails, while many heavier patients never do. However, weight gain, forefoot loading, and soft-tissue bulk can contribute to the mechanical environment around the nail.
7. Nail shape and nail-fold anatomy are important
Some patients have a nail plate that is naturally more curved from side to side. Others have prominent lateral nail folds or bulky soft tissue around the nail. These anatomical differences may increase the chance of nail–fold conflict.
This is clinically important because treatment should match the underlying problem. If the main issue is a narrow sharp nail edge, a nail procedure may be enough. If the main problem is excessive soft tissue, procedures that address the nail fold may be considered in selected cases.
Modern surgical reviews often divide treatment strategies into procedures that primarily target the nail plate/matrix and procedures that target the periungual soft tissue envelope. This distinction is useful because not all ingrown toenails are anatomically identical.
Staging: why severity matters
Ingrown toenails are commonly staged clinically, although staging systems vary. A practical approach is:
Mild ingrown toenail
The nail fold is tender and mildly inflamed, but there is no major infection, no significant discharge, and no large granulation tissue. The nail edge may be irritating the skin but has not created a severe chronic wound.
Moderate ingrown toenail
There is more obvious pain, swelling, redness, discharge, or local infection. The nail edge may be embedded in the skin. Conservative care may still work in selected cases, but recurrence is more likely.
Severe or chronic ingrown toenail
There is persistent pain, recurrent infection, hypergranulation tissue, bleeding, significant swelling, or repeated recurrence after self-care. At this stage, definitive treatment usually requires removing the offending nail edge and preventing that same edge from regrowing.
Severity matters because conservative treatment may be reasonable for mild cases, but repeated conservative care for a chronic, infected, recurrent ingrown toenail can prolong symptoms unnecessarily.
Conservative treatment: when surgery may not be needed
Conservative treatment is usually most appropriate for early, mild, or first-episode ingrown toenails, especially when there is no significant infection, no large granulation tissue, and no history of repeated recurrence.
The goal is to reduce pressure between the nail edge and the nail fold while the nail grows forward.
1. Footwear modification
Footwear advice is simple but important. Patients should avoid shoes that squeeze the toes together or press down on the nail. A wider toe box, softer upper, or temporary use of open footwear may reduce symptoms.
This does not “cure” every ingrown toenail, but it reduces the external pressure that keeps aggravating the nail fold.
2. Correct nail-cutting advice
The general advice is to cut the nail so that the front edge remains visible and not buried deep into the corners. Patients should avoid cutting aggressively down the sides, especially with sharp instruments.
The aim is not to create a perfectly straight nail in every case, but to avoid leaving a sharp side spike. If a painful spicule is present, professional removal is often safer than repeated digging by the patient.
3. Cotton-wick or dental-floss packing
In mild cases, a small piece of cotton or dental floss may be placed under the nail edge to lift it away from the skin. This can reduce pressure and allow the nail to grow forward.
A paper on cotton nail casting described this as a simple conservative approach for mild nail embedding, with reported pain improvement in many cases, although this type of evidence is not as strong as large randomized controlled trials (Gutiérrez-Mendoza et al., 2015).
The limitation is that packing methods require careful placement, regular monitoring, and patient compliance. They are less suitable when the nail fold is very inflamed, infected, bleeding, or covered by granulation tissue.
4. Gutter splinting
Gutter splinting involves placing a small splint between the nail edge and the nail fold. The splint acts as a physical barrier, preventing the nail edge from cutting into the skin.
This can be useful in selected mild to moderate cases. However, like cotton packing, it depends on the severity of the deformity, the amount of inflammation, and whether the patient can tolerate the splint.
5. Orthonyxia or nail bracing
Orthonyxia uses a brace to alter the curvature or loading of the nail plate. The principle is similar to orthodontics: instead of removing part of the nail, the brace applies a corrective force to reduce pressure at the nail edges.
This may be useful in selected patients with curved nails, recurrent mild nail-fold irritation, or those who wish to avoid surgery. However, the evidence base for bracing is still less robust than for partial nail avulsion with matricectomy in recurrent cases.
6. Managing infection and inflammation
If there is local inflammation, clinicians may recommend wound care, antiseptic soaks, dressing changes, or topical treatment depending on the presentation.
Antibiotics are not automatically required for every painful, red ingrown toenail. If the problem is caused by a nail spike acting like a foreign body, the key treatment is often to remove the offending nail edge. Antibiotics may be needed if there is spreading cellulitis, systemic illness, immunocompromise, diabetes-related risk, or more severe infection.
The important principle is source control. A persistent nail spicule can keep driving inflammation even if antibiotics temporarily reduce bacterial load.
Surgical treatment: when definitive treatment is needed
Surgical treatment is usually considered when there is:
- recurrent ingrowing;
- significant pain;
- infection that keeps returning;
- hypergranulation tissue;
- failure of conservative care;
- a clear nail spicule embedded in the fold;
- difficulty walking, training, or wearing shoes;
- chronic symptoms affecting work, school, or sport.
The aim of surgery is not simply to remove the painful piece of nail. The real aim is to prevent the same painful nail edge from regrowing.
Partial nail avulsion
A partial nail avulsion removes the offending side portion of the nail. This is usually performed under local anaesthetic.
The advantage is immediate removal of the painful nail edge. The disadvantage is that, if the nail matrix is left intact, the same nail edge may regrow and the problem may recur.
For this reason, partial nail avulsion alone is usually less definitive than partial nail avulsion combined with matricectomy.
Matricectomy: preventing the problem edge from regrowing
The nail matrix is the growth tissue that produces the nail plate. If only the nail is removed, it grows back. If the relevant part of the matrix is destroyed or removed, that portion of the nail should not regrow.
A matricectomy may be:
- chemical, using agents such as phenol, sodium hydroxide, or trichloroacetic acid;
- surgical, by excising the matrix tissue;
- combined, using surgical and chemical methods.
The 2023 systematic review by Exley et al. found that adding phenol to nail avulsion appears to reduce recurrence, although the authors also stressed that many studies were of limited quality (Exley et al., 2023a).
Chemical matricectomy: phenol, sodium hydroxide and TCA
Phenol matricectomy
Phenol is one of the most widely used chemical agents for ingrown toenail surgery. It chemically destroys the relevant part of the nail matrix after the offending nail edge has been removed.
The advantages of phenol include:
- low recurrence when performed correctly;
- relative technical simplicity;
- usefulness in inflamed or infected-looking nail folds;
- long history of use.
The disadvantages include:
- postoperative drainage;
- chemical tissue injury;
- delayed healing in some cases;
- need for careful application to avoid excessive tissue damage.
A 2022 systematic review and meta-analysis specifically evaluating phenol-based partial matricectomy concluded that phenol-based matricectomy is an established and effective treatment for onychocryptosis (Vinay et al., 2022).
How long should phenol be applied?
Phenol application time is a practical question. Too little phenol may risk recurrence. Too much may prolong healing or drainage.
Muriel-Sánchez et al. (2021) performed a randomized double-blind clinical trial comparing phenol application times. They reported that 30 seconds of phenol application had a shorter healing time than 60 seconds without reducing effectiveness in their study (Muriel-Sánchez et al., 2021).
This does not mean every clinician should automatically use 30 seconds in every case. Technique, concentration, exposure, tissue preparation, haemostasis, and case selection all matter. But the study supports the idea that shorter phenol exposure may reduce postoperative morbidity without necessarily increasing recurrence.
Sodium hydroxide matricectomy
Sodium hydroxide is another chemical matricectomy agent. It is used by some clinicians as an alternative to phenol. Some studies suggest it may have comparable recurrence outcomes, with potentially different healing profiles.
A 2025 retrospective study comparing surgical and chemical matricectomy found no statistically significant difference in healing time or prolonged pain between surgical, sodium hydroxide, and phenol matricectomy. The lowest recurrence pattern was observed in combined surgical and chemical approaches, followed by sodium hydroxide, then phenol, but the differences were not statistically significant (Acar et al., 2025).
This suggests that sodium hydroxide is a reasonable chemical option, but it does not clearly displace phenol as the universal standard.
Trichloroacetic acid
Trichloroacetic acid, or TCA, is another chemical cauterant used for partial matricectomy. A 2020 systematic review and network meta-analysis compared TCA, phenol, and sodium hydroxide and reported that TCA appears comparable to phenol for reducing recurrence (Chang and Lin, 2020).
TCA may be attractive because some studies suggest favourable healing or pain profiles. However, the available evidence is still not strong enough to claim that TCA is definitively superior to phenol or sodium hydroxide across all patients.
Surgical matricectomy and soft-tissue procedures
Chemical matricectomy is common, but it is not the only approach. Some procedures surgically remove the matrix horn. Others address hypertrophic or excessive nail-fold tissue.
This distinction is important. In some patients, the nail edge is the main offender. In others, the soft tissue fold is prominent and repeatedly rides over the nail edge. In chronic cases with large granulation tissue, soft-tissue management may be an important part of treatment.
Procedures described in the literature include:
- wedge resection;
- Winograd-type procedures;
- Zadik-type procedures;
- Vandenbos-type soft-tissue procedures;
- aesthetic reconstruction techniques;
- partial nail avulsion with chemical matricectomy.
The best procedure depends on the anatomy, severity, recurrence history, clinician experience, and the patient’s goals regarding healing time and nail appearance.
What does the highest-level evidence say?
The most important recent evidence comes from the two-part systematic review and meta-analysis by Exley et al. in the Journal of Foot and Ankle Research.
Recurrence and symptom relief
Part I reviewed randomized controlled trials on surgical treatment and found evidence that phenolisation reduces recurrence when added to nail avulsion. However, the authors were cautious because of limitations in trial quality, heterogeneity, and reporting (Exley et al., 2023a).
Healing time, pain, complications and satisfaction
Part II examined healing time, postoperative complications, pain, and patient satisfaction. It concluded that, despite many trials, few firm conclusions could be drawn because much of the evidence was low quality or poorly reported (Exley et al., 2023b).
This is a crucial point. The fact that many procedures exist does not mean they are all equally well proven. It also does not mean clinicians should ignore experience. Instead, it means that treatment decisions should combine:
- best available evidence;
- anatomical assessment;
- severity staging;
- recurrence history;
- patient preference;
- clinician skill and technique;
- expected healing time;
- cosmetic expectations;
- medical risk factors.
A practical treatment hierarchy
Early, mild ingrown toenail
For a mild first episode, conservative care is reasonable. This may include footwear changes, correct nail cutting, reduction of pressure, professional removal of a small spicule, cotton packing, gutter splinting, or bracing.
The goal is to break the pressure–inflammation cycle before the nail fold becomes chronically damaged.
Moderate ingrown toenail
For moderate cases, the decision is more nuanced. Conservative care may still be attempted, but if there is clear nail penetration, recurrent discharge, or significant pain, a partial nail avulsion may be more appropriate.
If recurrence risk is high, partial nail avulsion with matricectomy should be discussed.
Recurrent or severe ingrown toenail
For recurrent, severe, infected, or hypergranulating cases, the literature supports definitive treatment. In most cases this means removing the offending nail border and preventing regrowth of that same problematic edge.
Partial nail avulsion with chemical matricectomy, especially phenolisation, remains one of the best-supported options for reducing recurrence (Exley et al., 2023a; Vinay et al., 2022).
Common misconceptions
“The nail just needs to be cut out.”
Removing the painful nail corner may help temporarily, but if the same nail edge grows back, recurrence is common. This is why recurrent cases often need treatment of the nail matrix.
“Antibiotics will cure it.”
Antibiotics may help when there is spreading infection, but they do not remove a nail spike or correct the mechanical conflict. If the nail edge remains embedded, the inflammation may return.
“All ingrown toenails need surgery.”
Mild early cases may respond to conservative care. Surgery is more appropriate when the condition is recurrent, severe, infected, or structurally driven.
“Phenol is outdated.”
Phenol remains well supported in the literature, especially for recurrence prevention. However, sodium hydroxide and TCA are legitimate alternatives, and the ideal chemical agent may depend on clinician experience and patient-specific factors.
“The problem is always the patient cutting the nail badly.”
Poor nail cutting is common, but it is not the whole story. Footwear, nail curvature, sport, sweating, soft-tissue anatomy, trauma, and body mechanics may all contribute.
When patients should seek professional care
Patients should seek professional assessment if:
- pain persists for more than a few days;
- there is pus, bleeding, or increasing redness;
- the toe is too painful for normal shoes;
- the problem keeps recurring;
- there is hypergranulation tissue;
- the patient has diabetes, poor circulation, immune compromise, or neuropathy;
- self-treatment has involved repeated digging into the nail edge.
Patients with diabetes, vascular disease, or reduced sensation should be especially cautious. In these patients, even a small nail-fold wound may carry greater risk.
Conclusion
Ingrown toenails are common, but they are not always simple. The best current understanding is that they develop from a mechanical conflict between the nail plate and surrounding soft tissue. This conflict may be driven by nail-cutting technique, footwear pressure, trauma, sport, sweating, body weight, nail curvature, and nail-fold anatomy.
Mild cases may respond to conservative treatment, especially when managed early. However, recurrent or severe cases often require definitive treatment of the offending nail border. The strongest evidence supports partial nail avulsion combined with matricectomy, particularly phenolisation, for reducing recurrence. Sodium hydroxide and trichloroacetic acid are also supported by some comparative evidence, but the literature does not yet prove one chemical agent is clearly superior in all situations.
For clinicians, the key is to avoid treating every ingrown toenail as the same condition. A painful early nail-fold irritation, a teenage sports-related nail spicule, a chronic hypergranulating nail fold, and a recurrent post-surgical nail spike may all require different strategies.
For patients, the key message is this: if the problem is recurrent, infected, or repeatedly painful, it is usually not enough to keep cutting the corner out. The underlying nail–fold conflict needs to be properly assessed and treated.
References
8. Vinay, K., Narayan Ravivarma, V., Thakur, V., Choudhary, R., Narang, T., Dogra, S. and Varthya, S.B. (2022) ‘Efficacy and safety of phenol-based partial matricectomy in treatment of onychocryptosis: a systematic review and meta-analysis’, Journal of the European Academy of Dermatology and Venereology, 36(4), pp. 526–535.
Disclaimer: The word "treatment" in this article refers to the care and management of a patient’s health to prevent, cure, or improve a condition. Treatment results vary and do not necessarily indicate a cure. This article is for informational and educational purposes only and does not constitute medical advice.
Written and prepared by:
Mark Reyneker
Disclaimer: The word "treatment" in this article refers to the care and management of a patient’s health to prevent, cure, or improve a condition. Treatment results vary and do not necessarily indicate a cure. This article is for informational and educational purposes only and does not constitute medical advice.
Written and prepared by:
Mark Reyneker
B.T. Pod (SA), MSc (SA)
Podiatrist and Human Gait Specialist
Registered with the Podiatry Association of Singapore
Founder and Director:
Family Podiatry Centre Pte Ltd
Family Podiatry Centre Sdn Bhd
Solescape Orthotics Laboratory
Solescape Shoes brand
Recommended posts

