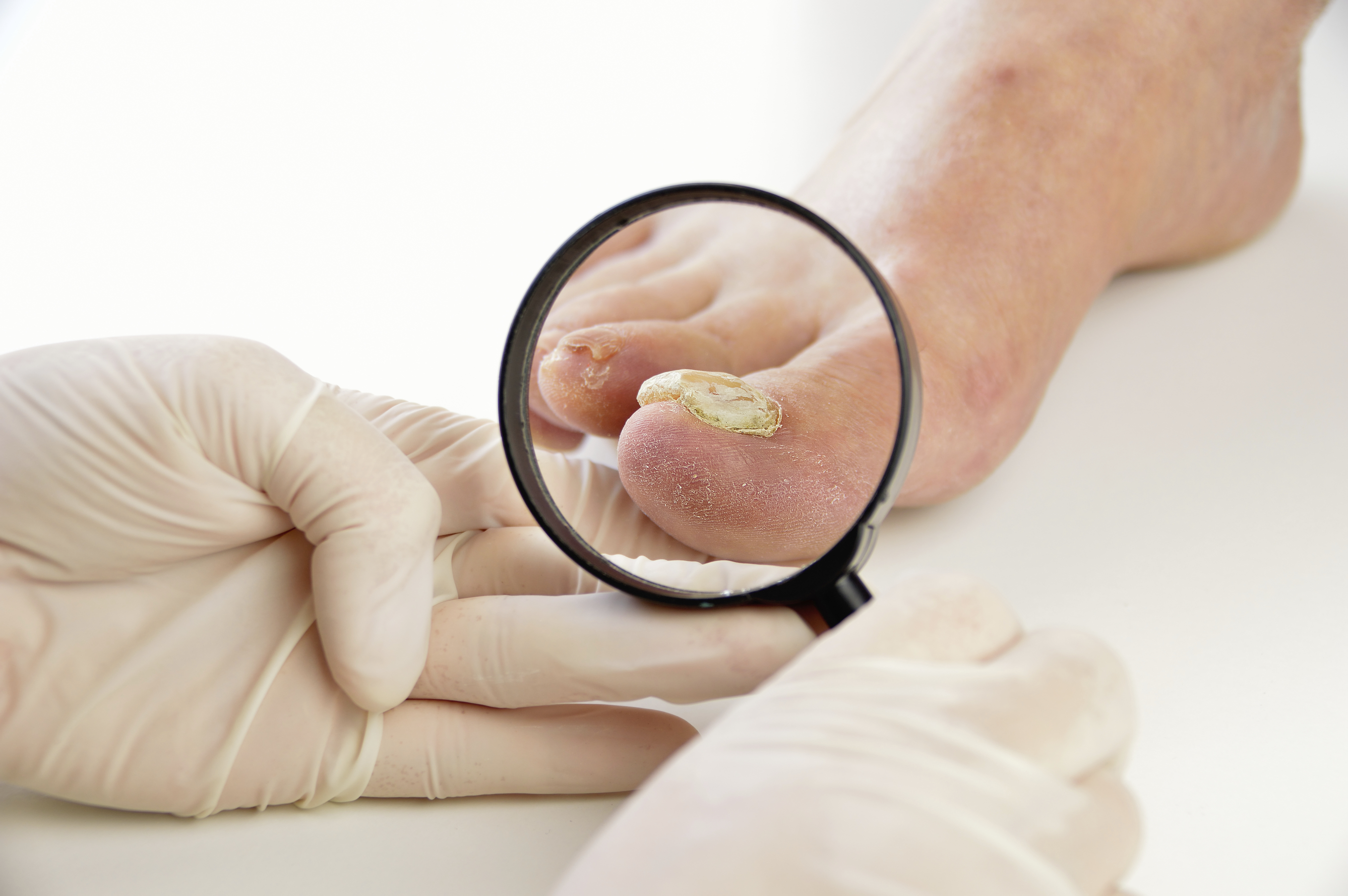
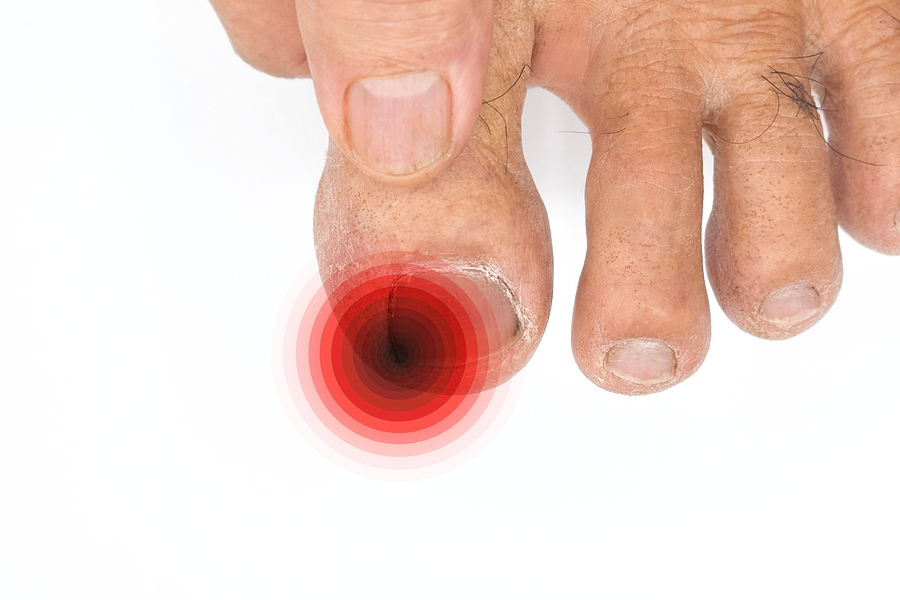
Why Urea Creams Are So Helpful for Dry Skin on the Legs and Feet
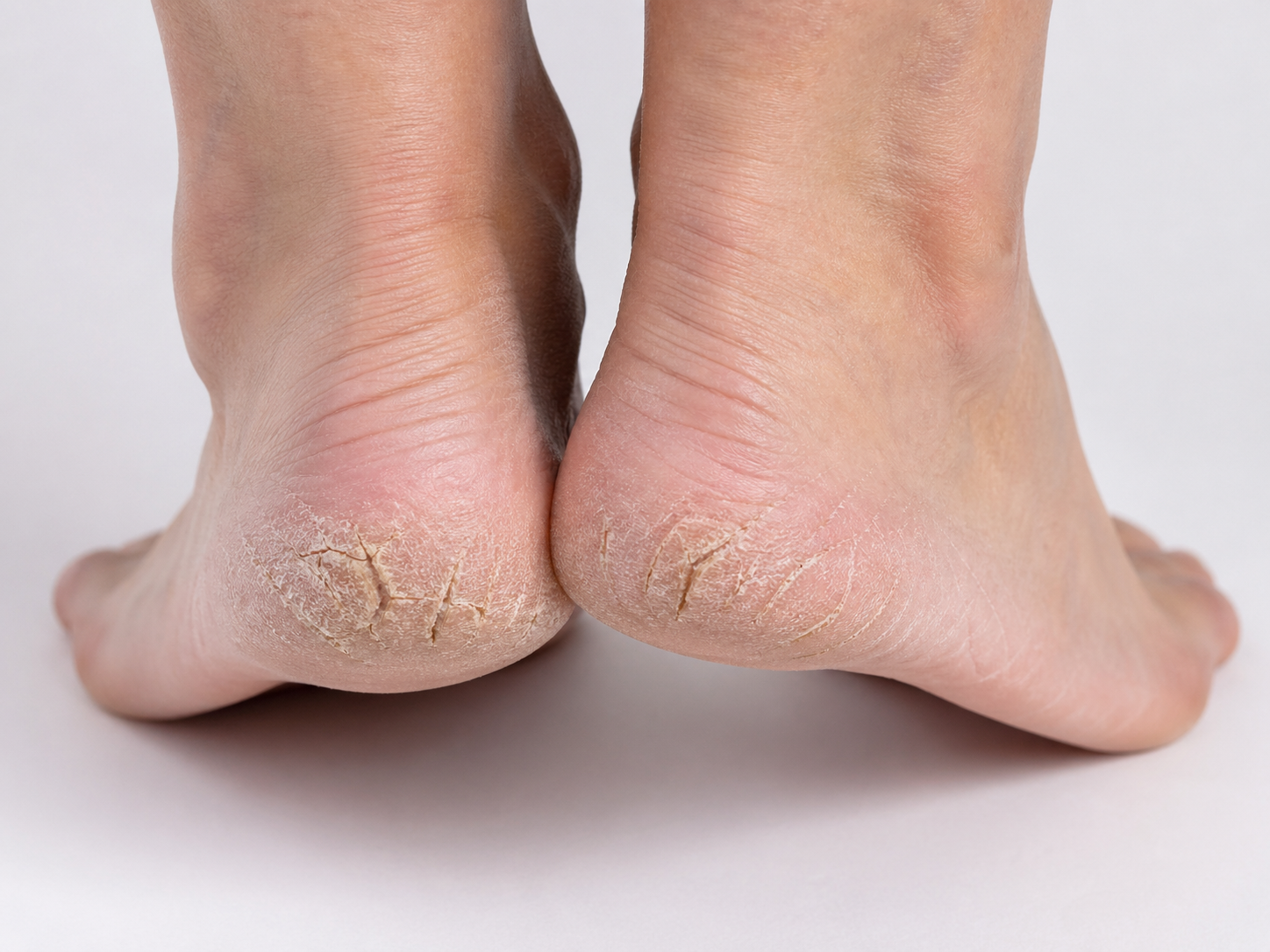
Dry, rough skin on the legs and feet is common. Many people notice flaking, scaling, tightness or cracked heels and assume it is simply a cosmetic issue. In reality, dry skin can reflect an impaired skin barrier, reduced water content in the outer skin layer and, in more severe cases, an increased tendency toward fissuring and discomfort. On the feet, this matters even more because the skin is exposed to repeated pressure, friction and weightbearing every day. Urea is one of the best-studied ingredients used in moisturising creams for this problem, particularly when dryness affects the heels, soles and lower legs (Barco and Giménez-Arnau, 2008; Parker, Scharfbillig and Jones, 2017; Piquero-Casals et al., 2021).
What is urea?
Urea is a substance that naturally occurs in healthy skin as part of what is known as the natural moisturising factor. In skincare and medical creams, urea is used because it helps the skin hold onto water, improves skin softness and, at the right concentrations, helps loosen areas of built-up, thickened skin. That combination makes it especially useful for the feet, where dryness and thickened skin often occur together rather than separately (Dirschka, 2020; Piquero-Casals et al., 2021).
What is xerosis?
Xerosis is the medical term for abnormally dry skin. It is more than skin that merely “needs lotion.” Xerosis is associated with disruption of the skin barrier, reduced hydration in the stratum corneum and altered skin lipids and natural moisturising factors. Clinically, xerosis often appears as rough, flaky, scaly or sometimes itchy skin. In more advanced cases, the skin can become less elastic and begin to crack (Barco and Giménez-Arnau, 2008; Amin et al., 2021).
What is hyperkeratosis?
Hyperkeratosis refers to abnormal thickening of the outermost layer of the skin, the stratum corneum. On the feet, this commonly appears as callus. It usually develops as a response to repeated pressure and friction. In simple terms, when one part of the foot is overloaded over time, the skin responds by producing more keratin as a protective mechanism. This is why plantar hyperkeratosis is often associated with altered pressure distribution, foot deformity and localized overload during standing and walking (Martínez-Nova et al., 2023; Spink et al., 2009).
What are dry dermatoses?
The term dry dermatoses is a broad clinical term rather than a single diagnosis. It refers to skin conditions in which dryness, roughness, scaling and barrier dysfunction are prominent features. Xerosis is one example, but similar changes are also seen in conditions such as atopic dermatitis, ichthyosis and some forms of psoriasis. Urea is widely used in dermatology because it can be useful across this broader group of dry, scaly skin disorders, not only in simple age-related or environmental dry skin (Dirschka, 2020; Piquero-Casals et al., 2021).
Why urea is particularly useful
Urea is valuable because it does several useful things at once. At lower concentrations, it mainly acts as a humectant, drawing and holding water in the outer skin. It also has emollient effects, helping dry skin feel smoother and more supple. At higher concentrations, it becomes more keratolytic, which means it helps soften and break down excess keratin in thick, rough or callused skin. This is particularly relevant for heels and soles, where a simple moisturizer may not be enough if the skin is both dry and thickened (Dirschka, 2020; Piquero-Casals et al., 2021).
Beyond surface hydration, urea appears to have biological effects on the skin barrier itself. Experimental work in humans has shown that urea can enhance barrier function and antimicrobial defence by regulating epidermal gene expression, including genes involved in keratinocyte differentiation and barrier formation. This helps explain why urea is often more effective than a basic cosmetic moisturiser when skin is genuinely dry, scaly and barrier-impaired (Grether-Beck et al., 2012).
Why the feet often need something more than a standard moisturizer
The skin on the soles and heels is naturally thicker than the skin on most other parts of the body. It also has to tolerate repeated loading, walking friction and footwear pressure. Because of this, foot skin often develops a combination of xerosis plus hyperkeratosis. That combination is important. Skin that is dry becomes less flexible, and skin that is thickened becomes less pliable. Together, these changes can make the heel or forefoot more vulnerable to painful splitting and fissuring. This is one reason urea-containing creams are so often recommended for the feet rather than ordinary body lotion alone (Parker, Scharfbillig and Jones, 2017; Piquero-Casals et al., 2021).
What does the research show?
The strongest clinical evidence is for foot xerosis, especially in people with diabetes. In a prospective, randomized, controlled, double-blind study, Pham and colleagues found that a moisturizer containing 10% urea and 4% lactic acid improved moderate-to-severe xerosis of the feet in patients with diabetes better than vehicle alone over four weeks (Pham et al., 2002).
Jennings and colleagues also reported benefit in a randomized, double-blind clinical study of foot xerosis, showing improvement with a salicylic acid and urea preparation compared with ammonium lactate treatment. This supports the clinical usefulness of urea-containing formulations for dry, rough foot skin (Jennings et al., 1998).
In another study, Ademola and colleagues found that 40% urea cream outperformed 12% ammonium lactate on several clinical and instrumental measures of xerosis. This finding is especially relevant when skin is not just dry, but also thickened and hyperkeratotic, because stronger urea preparations may provide additional benefit in those tougher cases (Ademola et al., 2002).
A systematic review focused specifically on foot xerosis concluded that urea-containing products are among the most researched topical treatments for dry feet. The review also noted that although the literature is somewhat heterogeneous, urea remains one of the best-supported active ingredients in this area of foot care (Parker, Scharfbillig and Jones, 2017).
What is urea cream good for?
In practical terms, urea-containing creams are especially useful for:
dry, flaky skin on the legs; rough heels; callused soles; cracked skin associated with xerosis; and dry skin conditions in which the barrier function is impaired.
Depending on the concentration, urea may be used primarily to hydrate mildly dry skin or to soften thicker, harder areas of hyperkeratosis. This flexibility is one of the reasons it has remained such a mainstay in dermatology and podiatric skin care (Dirschka, 2020; Piquero-Casals et al., 2021).
The bottom line
Urea is not just another moisturizing ingredient. It is one of the most clinically useful agents for dry skin because it addresses several parts of the problem at once. It improves hydration, supports barrier recovery and helps soften thickened keratin. For the legs, this can help with rough, dry skin. For the feet, where dryness and callus often overlap, it can be especially effective. That is why urea-containing creams are so commonly recommended for xerosis, dry heels and hyperkeratotic foot skin (Grether-Beck et al., 2012; Parker, Scharfbillig and Jones, 2017; Piquero-Casals et al., 2021).
Where Can You Buy Urea Cream for the Legs and Feet
The Family Podiatry Centre sells different type of urea creams that can be purchased over-the-counter. If your skin has thickened to the point of fissuring then a consultation can also be booked for further management of the condition.
Disclaimer: The word "treatment" in this article refers to the care and management of a patient’s health to prevent, cure, or improve a condition. Treatment results vary and do not necessarily indicate a cure.
References
8. Piquero-Casals, J., Morgado-Carrasco, D., Granger, C., Trullàs, C., Jesús-Silva, A. and Krutmann, J. (2021) ‘Urea in dermatology: A review of its emollient, moisturizing, keratolytic, skin barrier enhancing and antimicrobial properties’, Dermatology and Therapy, 11(6), pp. 1905–1915.
9. Spink, M.J., Fotoohabadi, M.R., Wee, E., Hill, K.D., Lord, S.R. and Menz, H.B. (2009) ‘Distribution and correlates of plantar hyperkeratotic lesions in older people’, Journal of Foot and Ankle Research, 2, 8
Written and prepared by:
Mark Reyneker
Written and prepared by:
Mark Reyneker
B.T. Pod (SA), MSc (SA)
Podiatrist and Human Gait Specialist
Registered with the Podiatry Association of Singapore
Founder and Director:
Family Podiatry Centre Pte Ltd
Family Podiatry Centre Sdn Bhd
Solescape Orthotics Laboratory
Solescape Shoes brand